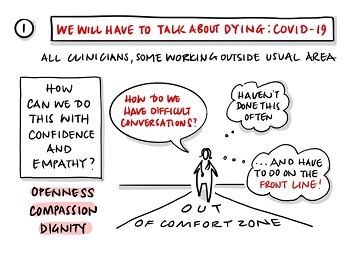
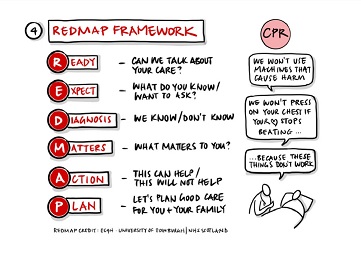
As a social service worker, or someone who is caring for others, you may experience death, dying and bereavement during the current COVID-19 outbreak.
We know this is an incredibly difficult time. As a key worker you may be feeling anxious or worried about your own family as well as the people you support, your colleagues and yourself. We also know that your existing experience will help you lead the way in providing compassionate, person-centred care and support even in these most challenging circumstances.
During this outbreak new information is being produced all the time. Although designed to help, it can feel overwhelming. This guide brings together information to support you in delivering compassionate, person-centred palliative and end of life care. It aims to help you:
- understand and feel confident in your role
- know and use the skills you have for facilitating conversations about death, dying and bereavement
- create a supportive network with colleagues.
If you’re new to the workforce, please use this information and speak with colleagues if you need support. If you’re an existing social service professional, we hope there is information here to enhance your confidence and help you share learning with others.
This guide is derived from the SSSC and NHS Education for Scotland's (NES) Palliative and End of Life Care (PEOLC) resources and accompanying guidance toolkit (eBook). We also want to thank the following partners who have contributed to this resource: Northern Ireland Social Care Council (NISCC), NHS Education for Scotland, Dr Paul Baughan, Open Change, The NHS Scottish Quality and Safety Fellowship, Dr Lara Mitchell, Dr Caroline Cochrane, Scottish Care, Healthcare Improvement Scotland, Professor Mark Williams and Scottish Partnership for Palliative Care.
Select 'Watch Video' below for a video from NISCC about holding onto hope in challenging times.